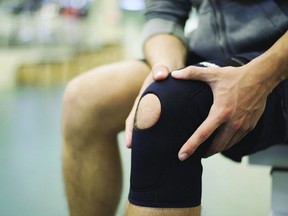
Study looks at whether tiny particles from period blood — which is easy to collect, non-invasive, and naturally regenerative — could help repair damaged cartilage
Published May 03, 2026 • 4 minute read
Reviews and recommendations are unbiased and products are independently selected. Postmedia may earn an affiliate commission from purchases made through links on this page.
Advertisement 2
THIS CONTENT IS RESERVED FOR SUBSCRIBERS ONLY
Subscribe now to read the latest news in your city and across Canada.
- Unlimited online access to articles from across Canada with one account.
- Get exclusive access to the Toronto Sun ePaper, an electronic replica of the print edition that you can share, download and comment on.
- Enjoy insights and behind-the-scenes analysis from our award-winning journalists.
- Support local journalists and the next generation of journalists.
- Daily puzzles including the New York Times Crossword.
SUBSCRIBE TO UNLOCK MORE ARTICLES
Subscribe now to read the latest news in your city and across Canada.
- Unlimited online access to articles from across Canada with one account.
- Get exclusive access to the Toronto Sun ePaper, an electronic replica of the print edition that you can share, download and comment on.
- Enjoy insights and behind-the-scenes analysis from our award-winning journalists.
- Support local journalists and the next generation of journalists.
- Daily puzzles including the New York Times Crossword.
REGISTER / SIGN IN TO UNLOCK MORE ARTICLES
Create an account or sign in to continue with your reading experience.
- Access articles from across Canada with one account.
- Share your thoughts and join the conversation in the comments.
- Enjoy additional articles per month.
- Get email updates from your favourite authors.
THIS ARTICLE IS FREE TO READ REGISTER TO UNLOCK.
Create an account or sign in to continue with your reading experience.
- Access articles from across Canada with one account
- Share your thoughts and join the conversation in the comments
- Enjoy additional articles per month
- Get email updates from your favourite authors
Article content
A new study published in Scientific Reports is turning something most people think of as a nuisance into a potential breakthrough for millions living with osteoarthritis. And, while it’s early, experts say it’s worth paying attention to.
Article content
Article content
Researchers in Lithuania looked at whether tiny particles from menstrual blood could help repair damaged cartilage. These particles, called extracellular vesicles (EVs), act like messengers between cells, helping regulate inflammation and tissue repair. In this case, they were taken from menstrual blood-derived stromal cells and tested on cartilage samples from women with osteoarthritis.

Idea taps into huge unmet need
More than 600 million people worldwide have osteoarthritis, and current treatments don’t actually fix the problem — they mostly just dull the pain.
“Currently, there are no approved disease-modifying therapies for the treatment of osteoarthritis,” said Dr. Mohit Kapoor, co-director of UHN’s Schroeder Arthritis Institute, in comments to the Toronto Sun. “The approved therapeutics … only provide symptom relief … without stopping the underlying disease pathology.”
By signing up you consent to receive the above newsletter from Postmedia Network Inc.
Article content
Advertisement 3
Article content
That’s where this research stands out
In lab and tissue experiments, the menstrual blood-derived EVs (MenSC-EVs) appeared to “stimulate cartilage cells called chondrocytes and promote cartilage matrix production,” Dr. Kapoor explained. In simple terms, they nudged damaged cartilage cells to start rebuilding.
The Lithuanian team saw similar results. Their experiments showed the EVs boosted extracellular matrix (ECM) production — the structural “scaffolding” that gives cartilage its strength — while also slowing down tissue breakdown.
Therapy worked on cartilage ‘from postmenopausal women’
Even more striking, the therapy worked on cartilage from older, postmenopausal women, where natural repair ability is usually much weaker.
“What surprised us most was that the therapy worked even in cartilage cells from older postmenopausal women,” said Dr. Ilona Uzielienė, a researcher at KTU Faculty of Chemical Technology, in a press release.
Advertisement 4
Article content
The EVs also increased progesterone receptor expression in aging cartilage cells, hinting at a possible hormone-linked repair mechanism. The study notes this could be especially important in post-menopausal osteoarthritis, where hormone changes play a role in disease progression.
Vesicles did more than just block damage
At a deeper level, the research showed these vesicles enhance anabolic activity — the “building up” side of cell function — rather than just blocking damage. They increased key cartilage genes, improved ECM density, and reduced markers of cartilage breakdown. Importantly, they did all this without triggering major inflammation, a critical safety consideration.
Dr. Kapoor called these findings encouraging, but emphasized they’re still early.
“While this is an … important advancement, it would be interesting to … investigate if this therapeutic strategy is able to reverse or halt cartilage damage in pre-clinical experimental models in vivo,” he said. In other words, it works in the lab — now it needs to prove itself in living systems.
Advertisement 5
Article content

Treatment could be easier to employ
There’s another twist: The therapy isn’t based on cells themselves, but on what they produce. That makes it a “cell-free” treatment, which could be safer and easier to use.
From a practical standpoint, menstrual blood has some clear advantages. It’s easy to collect, non-invasive, and naturally regenerative — these cells help rebuild the uterine lining every month. That gives them a built-in repair toolkit that researchers are now trying to repurpose.
Potential treatment’s challenges
Still, turning this into a real treatment isn’t straightforward. One major hurdle is delivery.
EVs are fragile and break down quickly, so researchers used “biological scaffolds” — protective structures that hold the vesicles in place and release them slowly when a joint moves.
Dr. Kapoor explained why that matters: “Biological scaffolds are typically used for drug delivery … to enhance stability, specificity and loading capacity of EVs.” But they come with challenges, including “loading and controlled release” and making sure the whole system is safe.
Advertisement 6
Article content
Lithuanian team echoed that concern
Designing these scaffolds is complex — they need to be chemically stable, mechanically strong, biologically compatible, and actually manufacturable at scale. According to the researchers, replicating cartilage, which has a very specific structure and handles constant stress, makes it even harder.
Even if those hurdles are cleared, there are bigger questions.
Dr. Kapoor pointed out that safety and consistency still need to be nailed down. “Further investigations and in vivo studies need to be performed to ensure they are safe and demonstrate potent regenerative properties,” he said, adding that “donor variability” — differences between individuals — also needs careful study.
Study acknowledges these gaps
So far, the results are based on in vitro and ex vivo experiments, meaning lab-grown cells and tissue samples — not full living organisms. Long-term effects, optimal dosing, and how the therapy behaves in the body are still big question marks.
Advertisement 7
Article content
There are also biological nuances. While EVs were quickly absorbed by cartilage cells and boosted repair signals, they didn’t significantly change cell growth or movement. That suggests they help restore balance rather than aggressively forcing regeneration — a potentially safer but slower approach.
Overall picture is promising
The researchers conclude that MenSC-EVs can stimulate cartilage repair, protect tissue, and avoid triggering harmful inflammation — all while being sourced in a non-invasive, renewable way. Compared to bone marrow-based therapies, that’s a big practical advantage.
Dr. Kapoor agrees the concept is worth pursuing, especially given how little progress has been made in actually reversing osteoarthritis.
“There is a tremendous effort happening around the globe to find ways to stop or reverse cartilage damage,” he said. “So far, we haven’t been successful in clinical trials.”
This study doesn’t change that — yet. But it does open a new door.
For more health news and content around diseases, conditions, wellness, healthy living, drugs, treatments and more, head to Healthing.ca – a member of the Postmedia Network.
Article content
.png)
 1 hour ago
11
1 hour ago
11



























/https%3A%2F%2Fsportsmole-media-prod.s3.gra.io.cloud.ovh.net%2Fuploads%2F2026%2F02%2Fimago1072832028-1-1-6996d086195c8904803070.jpg)
 Bengali (BD) ·
Bengali (BD) ·  English (US) ·
English (US) ·